What the Opioid Crisis Can Teach Us about the War on Drugs
America has seen a veritable explosion of serious drug abuse over the past two decades. In 1999, the year the Centers for Disease Control switched to a new system for tallying causes of death, Americans suffered fatal overdoses at a rate of six per 100,000. By 2015 the rate was 16 per 100,000, a total of over 50,000 deaths. In the official statistics that year, nearly two-thirds of drug overdoses involved an opioid of some kind—an undercount since many overdoses are not properly coded as opioid-related. Around 60 percent of the opioids on which users overdosed were illicit drugs like heroin, rather than (or in addition to) drugs sold legally with a prescription.
Nor is there any sign of a let-up. Official data for 2016 won’t be available until later this year, but preliminary numbers suggest that overdoses soared more than a fifth beyond the 2015 levels. We are witnessing the self-inflicted, if usually accidental, demise of tens of thousands of people each year—more Americans than die of gunshot wounds or injuries sustained in car accidents.
We are also watching the demise of a common way of looking at drug addiction. The journalist Sam Quinones, author of Dreamland (2015), a book chronicling the epidemic and the rise of Mexican heroin in the United States, described the shift in his own thinking in a podcast conversation with the economist Russ Roberts. Quinones said that when he was in Mexico reporting previous books and articles, he had believed
that all drug stories were demand-driven, and that drug scourges were created by demand for those drugs. Now, when I did this book, this changed my mind, honestly. I came to think that really most drug problems begin because of excess supply—easy, cheap availability of a drug. And that’s exactly what happened here.
To address the epidemic, it is imperative that we study how the supply of drugs rose. It is imperative that we study to whom, exactly, these drugs flowed.
If this were a story of legitimate patients getting hooked on the drugs they were prescribed—and only then beginning to abuse their pills and turning to illicit substitutes—then the problem would simply boil down to prescribing practices. Attacking the problem would have few ramifications for the broader debate about restrictions on drugs versus legalization, for if these abusers would never have taken drugs without a doctor’s say-so, there’s no reason to think they’d get hooked on a drug that is legal but strongly taxed, regulated, and discouraged.
But if, by contrast, the abusers of opioids are mainly individuals who abused them from the beginning, then the epidemic is a strong indicator of the consequences of entirely legalizing drugs. It is a demonstration of what happens when drugs are in full supply, safely manufactured, and easily available to those seeking a high and at risk of addiction.
This Liberty Forum essay, after giving an overview of how the epidemic spread, will argue that the second scenario predominates. The facts suggest that a substantial share of the epidemic has occurred among people who began as non-medical users, which should prompt concern among those who have held romantic notions (as I have) about drug legalization.
The War on Drugs, or at least on hard drugs, has not been as ineffective as many think. True, “war” is a terrible metaphor, because it is not something we can ever win. Rather, it’s a continuous effort that reduces drug abuse relative to what it would otherwise be by raising the costs of using drugs. That said, those opposed to even the legalization of marijuana at this point have to admit that the public is not on their side. Support for marijuana legalization has crossed the 50 percent threshold.
When it comes to legalizing hard drugs, the case is otherwise: Very few Americans are in favor. Therefore our thinking should shift to how best to control the flow of lethally addictive substances, prevent addiction, and treat addicts. This means reforming the War on Drugs rather than ending it. The task for the future is to focus the most punitive aspects of the criminal justice system on dealers while using scientifically tested techniques to help addicts get better.
Overview
The story begins in the 1970s, when the medical profession came to recognize that it had done a poor job of controlling pain. The effort began with the terminally ill, who were now given palliative care instead of being forced to die in agony. In 1986, the World Health Organization promoted a “ladder” approach for cancer patients in which doctors would start with milder medications but would continuously increase their potency until the pain was controlled. It was deemed a secondary concern that people might become addicted on their deathbeds.
In the late 1980s an effort began to extend this approach to chronic pain, a symptom that is notoriously hard to measure accurately. Few would deny that for many patients, pain is real and can devastate their quality of life. Prominent medical organizations, and others, argued that opioid painkillers, which are chemically similar to heroin, could be used safely for long periods of time with minimal risk of addiction. They often cited a brief 1980 study from the New England Journal of Medicine—I say study, but it was in fact a five-sentence letter to the publication’s editor. In this letter, a doctor and his assistant at the Boston University Medical Center reported that they had analyzed a database available to them and that, of 11,882 people given narcotics while hospitalized, only four showed signs of addiction, only one of which was severe.
In what has to be one of the most consequential episodes of confirmation bias in modern history, the argument made by the doctor and his assistant in 1980 carried the day. By 1999, the Joint Commission on Accreditation of Healthcare Organizations had designated pain the “fifth vital sign” (alongside body temperature, pulse, respiration rate, and blood pressure). Patients were asked to rate their own pain on a scale of 1 to 10. Prescriptions were written based on those scores. Doctors, held hostage to customer-satisfaction surveys in which their patients were asked how well their pain had been controlled, had signed on to the new paradigm.
Unsurprisingly the pharmaceutical industry signed on, too. Of particular importance was Purdue Pharma’s introduction of OxyContin in 1996. OxyContin, manufactured to release the opioid oxycodone slowly over the course of a day, promised 12 hours of relief from chronic pain, and for the same reason it also promised a lower chance of addiction than other, similar painkillers. Purdue marketed the drug aggressively and sometimes dishonestly. (There were hundreds of millions of dollars in fines and settlements years later, with lawsuits continuing to this day.) Physicians wrote month-long prescriptions to patients who had undergone surgeries that almost certainly would not keep them hurting for that long.
These two factors working in conjunction—a medical profession eager to kill pain and a pharmaceutical industry eager to sell painkillers—proved deadly. The prescription of opioids skyrocketed in the United States in a way it didn’t anywhere else, and with the increased prescribing came increased addiction and overdosing. Some addicts sought prescriptions from multiple physicians at once. Others visited “pill mills,” cash-only businesses that were staffed by licensed (but shady) doctors who were there to hand out prescriptions with no questions asked. And addicts weren’t only swallowing the pills with a glass of water. Many crushed them up so they could be snorted, injected, or dissolved in a beverage, thus defeating the 12-hour release mechanism (which didn’t always last 12 hours anyway, it turned out) and getting the full effect immediately. For a long time, painkiller sales and fatal painkiller overdoses rose in nearly perfect conjunction.
A few years ago some legislators, doctors, and regulators started noticing there was a problem and began taking steps to fight it. Purdue released a new version of OxyContin in 2010 that was harder to crush and started monitoring its sales more closely. States started experimenting with prescription registries to prevent doctor-shopping and cracked down on the pill mills. Painkiller deaths did stop rising; Florida in particular saw success with its efforts to shut down pill mills. Overall prescribing fell, too, starting in 2010.
Heroin use, on the other hand, began to rise at this point as painkiller addicts switched to an alternative that was chemically similar, cheaper, and also far more dangerous. Though the percentage of opioid users who switched to heroin was low, it was enough to give the heroin market a substantial boost relative to where it started. Studies indicated that, in a striking contrast with previous eras, most users of heroin who began in the 2000s and 2010s had previously abused prescription drugs. Fatal heroin overdoses doubled between 2010 and 2012 and again between 2012 and 2015; in that final year there were about 13,000 of them in the official statistics, likely an undercount thanks to the coding issue I noted at the outset, with opioid overdoses not always being properly recorded as such.
Moreover, as the heroin market grew, the heroin being sold began to be laced with synthetic opioids (that is, those not derived from opium poppies) such as the highly lethal fentanyl. This once-obscure drug is used medically as an anesthetic, but the fentanyl mixed with heroin of which we now hear so much is normally procured from China through illegal trafficking. Meanwhile, even with the above-mentioned downturn in opioid prescriptions, enough of them are still written each year for every American adult to have one (though it’s worth noting that many of the prescriptions, especially those given after surgery, go unused).
Thus has the overall epidemic continued basically uninterrupted, with soaring heroin and fentanyl deaths canceling out any improvement regarding other opioids.
Who Has Fallen Victim?
Since 1999, opioid overdoses have risen in every state of the union and among every demographic. But it isn’t as though they are distributed within a perfect cross-section of America. It’s worth tallying where and whom the epidemic has hit hardest.
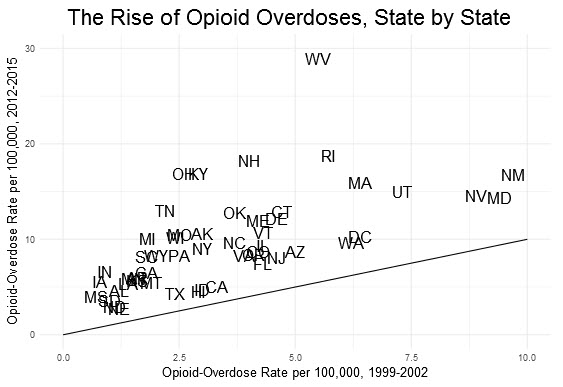
The most striking trend is geographical. Around the turn of the millennium, in states bisected by the Appalachian mountains—West Virginia, Kentucky, and Ohio—there were not out-of-the-ordinary rates of opioid deaths. The same was true of New Hampshire and Rhode Island in the Northeast. But in recent years, these are the states where the problem is the worst.
The chart below illustrates this. Each state is plotted according to its opioid-overdose rate around the turn of the century (the X axis) and in the most recent data available (the Y axis). West Virginia’s position is the most striking: It’s toward the middle horizontally but towers over all others vertically. Just as important, every single state saw its rate rise. If a state had had the same rate in both periods, it would fall on the black line toward the bottom of the chart. (Note that these are official statistics, and efforts to correct for underreporting indicate that many states, especially Pennsylvania and several in the South, should look worse than they do.)
The epidemic is also concentrated among low-income Americans, and among whites and Native Americans. Blacks have an overall rate of fatal drug overdoses that is about 40 percent lower than that of whites; the rate for Latinos is about 40 percent below that; and the rate for Asian Americans is less than half of that of Latinos (and 85 percent below whites’ rate). Opioid deaths have long been concentrated among the middle-aged but, in the past few years, young adults have been catching up thanks to heroin.
And now we arrive at the key question: Are we talking here about pain patients—those who have inadvertently become addicted, so much so that they eventually take a fatal dose? Or are these folks non-medical users, who got hooked through deliberate misuse?
Sorting out and quantifying the two categories is far from easy. Ideally we would have a trove of survey data bearing directly on the issue—but the nation’s largest surveys on drug use do not ask addicts how they originally became addicted. As a result, we need to consult smaller studies and use them to paint the bigger picture.
The most directly relevant piece of evidence I have been able to find, unfortunately, is a 2010 survey that asked a convenience sample of 75 hospitalized opioid addicts how they originally got hooked. The answer was that 41 percent said it started with a legitimate prescription; the rest had started with diverted prescriptions or with drugs they bought on the street. The results also indicated that addicts often moved from legitimate drugs to illicit sources if needed, because 92 percent of the addicts in the survey had used drugs from illicit sources at some point.
No one would call that study definitive, given its small sample and the fact that the participants were not chosen to be representative. But the other available evidence suggests the study’s finding is in the right ballpark. For instance, as the journalist Maia Szalavitz has pointed out, one study showed that only 13 percent of opioid-overdose visits to emergency rooms are by people with a medical diagnosis of chronic pain. Mental disorders were nearly three times as common in this group.
Also, the National Survey on Drug Use and Health suggests that only one-fifth of opioid abusers currently get their drugs from a single doctor; two-thirds get them from friends and relatives. In addition, before OxyContin was reformulated, more than half of those who abused it snorted it at least some of the time, and more than a third injected it. In many cases, these behaviors no doubt started after a legitimate prescription led to addiction, but they do illustrate that addicts are engaging in obvious abuse, rather than just taking pills they received through a prescription.
To be absolutely clear, 41 percent of addicts’ having started out as medical patients with legitimate prescriptions is hardly a small percentage, and there is plenty of evidence that some patients become addicted, especially if they have other risk factors such as mental illness or a history of drug abuse. A poll by the Washington Post and the Kaiser Family Foundation indicated that 31 percent of people who’d taken prescription painkillers for at least two months of the past two years said it would be (or was) “very hard to quit”; 23 percent thought they were (or had been) “addicted.”
A study published in the November 2015 issue of Pediatrics suggested that legitimate use of opioids in adolescence was associated with a 33 percent increased chance of misuse (though not necessarily addiction) later, and that the increase was concentrated among patients with little or no history of drug use. Another in the Annals of Internal Medicine found that even after patients had received hospital treatment for an overdose, they could get another prescription 90 percent of the time, perhaps because their doctors had no way of knowing about the overdose.
All of this means that the pharmaceutical and medical establishments will need to be part of any solution. Doctors must prescribe these pills less often without denying relief to people who really do suffer from extreme pain, as they have already started doing. They must also carefully warn patients of the risks, which they frequently still neglect to do (according to the aforementioned KFF/Washington Post poll). Drugmakers and sellers must continue to monitor their sales and to work on abuse-deterrent forms of these products or, better yet, must try to develop wholly new and less dangerous analgesics. States’ Medicaid programs, which are footing much of the bill for the opioid epidemic—paying for both the pills and the treatment—should carefully monitor where their money is going.
But since so much of the problem stems from blatantly illegal behavior rather than the misuse of legitimately prescribed drugs, our criminal justice system will also be involved. We must decide how much of the War on Drugs to keep and how much to change or discard.
Fighting the War
Before we discuss how the War on Drugs should change, we need to understand how it works now and how opioids fit in.
Drug offenders violate state and federal laws, and may find themselves in either system depending on the circumstances. As of 2015, about 300,000 people were serving drug sentences in America’s prisons, roughly two-thirds of them in state facilities. This amounted to 15 percent of all state prisoners and half of federal prisoners.
In 2012, the most recent year with detailed data available, 6.5 percent of federal drug prisoners were serving time for heroin offenses, with another 3.5 percent being punished in regard to drugs classified as “other,” a group that includes prescription painkillers. (More than half of the total were involved in the cocaine trade.) Inmate surveys conducted in 1997 and 2004 suggest that while the breakdown among the types of drugs is broadly similar in state and federal facilities, heroin offenders’ share of drug inmates tends to be higher in state prisons.
Taking a rough but educated guess, then, maybe 10 percent of drug prisoners today are serving time for opioids including heroin. In other words, at any given time, roughly as many people—about 30,000—are imprisoned for opioids as die from them in a year.
A popular misperception, meanwhile, is that America imprisons large numbers of people guilty of nothing more than drug possession. The federal system holds very few drug prisoners who weren’t involved in trafficking; in state prisons, only about one-quarter of drug prisoners were sentenced for possession. And consider that this is the case even though, almost by definition, drug users outnumber drug dealers many times over.
This isn’t because drug users don’t come into contact with the justice system. It’s because they are rarely sentenced to prison for their crimes, and usually serve very short sentences when they are. In fact, arrests related to possession are more than quadruple those related to dealing.
Another misperception is that drug users are garnering more sympathy now that a problem has emerged that is concentrated among white Americans, the evidence for this being the chorus of calls for treatment for opioid addicts. But the system, as I said, was already going light on users. The reality is that the American public has supported this two-track approach—incarceration for dealers, treatment for addicts—for decades.
As I have explained in The American Conservative, citing Barry Latzer’s The Rise and Fall of Violent Crime in America (2016), when the use of crack cocaine was at its height back in 1989, public opinion polls showed that Americans, by 57 percent to 33 percent, wanted to see addicts receive treatment rather than punishment. At the time the opioid epidemic hit in 2001, arresting users was again the least preferred policy according to the polls. (More favored measures were stopping importation, arresting domestic drug dealers, and heightening awareness of the problems of addiction.) Today, with drug deaths soaring, particularly among whites, Americans still are no more likely than before to express the opinion that the government does not devote enough resources to fighting addiction.
This is by way of emphasizing that the proposals that follow are really not so great a departure.
How to Curb the Use of Opioids
The effort to legalize drugs has seen groundbreaking success over the past decade but only with regard to marijuana. As mentioned, there is little public support for going further. Marijuana legalization is not consequence-free, to be sure. It drains users of their initiative and, notwithstanding its reputation, it is habit-forming. Be that as it may, Americans have come to see that pot simply isn’t worth locking people in cages over. The opioid epidemic therefore requires no great rethinking on this front. Indeed, for many, medical marijuana may be a superior alternative to opioids for pain relief. It is not as addictive as opioids and seldom if ever kills those who smoke it.
I will say it plainly: Because opioids enslave and destroy when not used correctly, they should not be fully legalized. Besides, while there’s nothing illogical about the libertarian belief that people should be allowed to take whatever risks they want in the interest of getting high, as a practical matter this is not a position that holds much sway with the public. A Vox/Morning Consult poll last year, as well as a Huffington Post/YouGov poll in late 2013, found negligible support for legalizing hard drugs. Support for heroin legalization was below 10 percent in each.
I believe that there are ways to reform the War on Drugs that would improve outcomes, be consistent with public opinion, and be a step in the right direction, even from a hardline libertarian perspective. What we should do is double down on the distinction between dealers and users. The former should be treated as criminals, as they are today; the latter, if they are willing, as candidates for treatment.
What are the optimal enforcement policies, and the optimal treatment methods?
Regarding enforcement, what is clear is that making a drug illegal instead of legal dramatically increases its price. (If marijuana were farmed conventionally and openly, for example, the price would fall something like 80 percent.) However, the evidence is quite unclear as to whether it would be worthwhile to step up enforcement of drug laws against dealers or whether, by contrast, we could relax enforcement or sentencing somewhat without endangering lives. As a 2014 review of the research put it: “The number of studies available is small; they use a great variety of outcome and input measures and they all face substantial conceptual and empirical problems.” So these kinds of changes are fertile ground for state-by-state experimentation.
Regarding treatment, we should have no illusions. Many addicts refuse help. We know of no treatment that is effective more than about half the time. And treatment is expensive. But when tens of thousands of people are dying each year, and many more are drawn into addiction and may represent the fatalities of the next decade, even a small improvement affects a lot of lives. Not only that, improvements however small can recoup at least some treatment costs by reducing future healthcare needs and crime and making addicts more employable.
Drug-addiction interventions are highly susceptible to the scientific method. This argues for randomly assigning addicts to different treatments and seeing what works best. The existing research underscores the effectiveness of two tactics in particular—repeated drug testing coupled with minor, immediate punishments to keep addicts on the straight and narrow, and medications that reduce cravings—and we should make a concerted effort to find additional approaches.
There are currently some 3,000 “drug courts” operating around the nation that specialize in punishing and monitoring low-level drug offenders. They’ve existed for about a quarter century, and work largely by requiring offenders to get treatment or go to jail. There are many criticisms one can make of drug courts in general. But researchers have stumbled upon a variation on the concept that actually works.
This approach is most commonly identified with a program called Hawaii’s Opportunity Probation with Enforcement (HOPE). The program’s key concept is “swift, certain, and fair.” Participants face random drug tests and if they fail, they are immediately given a small punishment such as a short jail stay. This avoids a common problem in the probation system, which is that offenders are repeatedly forgiven for small lapses until their overseers get fed up and send them to prison for a lengthy sentence. The data on HOPE indicate that it is far more effective than normal probation while it lasts, and that it reduces future drug charges and imprisonment as well. The results of similar programs elsewhere are also promising.
Addiction medications have proven to be highly effective, if far from 100 percent so. These include methadone, buprenorphine, and naltrexone. They work by satisfying cravings without getting the user high. One study showed that naltrexone reduced relapse rates from 64 percent to 43 percent, suggesting that it prevents one relapse for every five patients to whom it is prescribed.
The common knock against this approach is that it “replaces one drug with another.” This is true as a statement of fact, but it fails as an argument, for the simple reason that not all drugs are equally harmful. The difference among drugs is especially pertinent now that efforts are underway to control prescription-pill diversion, and heroin, after all an opioid itself, is the most readily available substitute for addicts. A more serious objection is that, as mentioned, drug treatment is expensive. Methadone and buprenorphine maintenance both cost in the ballpark of $4,500 a year; monthly naltrexone injections cost more than $1,000 each. (Localities have faced a similar issue with overdose-reversing drugs, with some floating the idea of refusing to revive addicts after a certain number of overdoses.)
Repeated drug testing coupled with minor punishments is a formula that several states are already pursuing. If this country is serious about controlling the epidemic and reducing drug abuse in general, this approach should be dramatically expanded. HOPE-style programs are still relatively new (HOPE itself began in 2004), and perhaps owing to the expense, medication-based treatments are unavailable to many. The Surgeon General estimates that only one in 10 Americans with a substance-use disorder receive specialty treatments, and also finds that too few physicians and treatment programs offer medications. (By one estimate, for example, half of the counties in California are “opioid treatment deserts.”) The Surgeon General further observes that medications have not even been developed for treating addictions to substances other than opioids and alcohol. Inside the justice system and out, then, there are ways to improve the situation if we’re willing to spend the money.
One final possible area for reform of our justice system deserves mention: “Harm reduction” techniques intended to help addicts get high safely, which oblige law enforcement to turn a blind eye. The classic example here is needle exchanges. Today, as Sally Satel of the American Enterprise Institute lays out in an excellent National Affairs essay on the opioid epidemic, Boston provides a “Supportive Place for Observation and Treatment” where those who’ve injected drugs can “ride out the high, be treated by nurses should complications develop, and, ideally, be persuaded to embark on a path to recovery.” In Canada, “Safe Consumption Sites” allow users to bring and abuse their own drugs “in the presence of nurses who can administer oxygen and naloxone [an anti-overdose drug] if needed.” As Satel says, the results of such efforts must be studied carefully, as there are substantial risks to public safety and public health involved. But small-scale experiments such as Boston’s should be encouraged.
In short, the opioid epidemic has dispelled a lot of myths and quashed a lot of hopes regarding the War on Drugs. Legalizing drugs looks much less wise than it once did and, in any event, has little chance of gaining public support. A much narrower, but still powerful, set of reforms is in order.