Australia's decision will do more to advertise the anti-vax position than quietly letting the tennis star play would have.
Learning from Epidemics Past
If the history of public health crises teaches us anything, it is often that the knowledge we have during the crisis itself is woefully insufficient when new challenges emerge. Covid-19 is just such a challenge. Scientists are struggling to understand the specific ways the virus attacks our immune systems, who are at the greatest risk, and how exactly it spreads. The difficulty is that whether we are prepared and prudent, any preparations would have been based on old and established ways of thinking. While in January the world was rapidly trying to produce ventilators, we know now that these devices seem to do little to prevent people from dying.
Humans require mental models to organize and understand the world. Social scientists have long known that we do not “objectively” approach the world in which we live. Whether you want to start more recently with Jonathan Haidt or go back to Herbert Simon, or even Adam Smith, those who examine human behavior in institutions have long understood that people have biases and heuristics that influence the way we behave in and analyze the world around us.
Thomas Kuhn’s monumental book, The Structure of Scientific Revolutions, applies this same mode of thinking to the scientific world. Kuhn argues that science is best understood as a collection of paradigms, models that help scientists understand the world around them. What Kuhn refers to as a “mature” science has periods of normal scientific pursuits within the dominant paradigm of a science. These paradigms guide research to answer questions raised by the existing paradigm. If research raises issues that cannot be explained by the existing paradigm, it is possible to have “revolutionary” science and the established paradigm can be replaced by newer paradigms that better explain the world. An obvious example of this would be Einstein’s work that overturned the Newtonian model of physics. Kuhn argues that this model of paradigms exists in all the mature sciences, including medicine and epidemiology. Interestingly, scientists can be so entrenched in an existing paradigm that it can take years before a new paradigm is eventually accepted and the community of scientists all come to accept it as reality.
Unfortunately, the history of public health is full of examples of how paradigmatic thinking based on faulty paradigms can lead to disastrous outcomes. Steven Johnson’s Ghost Map, a history of the 1854 cholera epidemic that killed more than 10% of the inhabitants of the Soho community in London, is a powerful illustration of how existing paradigms can blind scientists from seeing plainly the truth about the causes and cures of diseases.
You have probably never heard of the word miasma today, but in the 19th century it was the dominant paradigm in disease theory. Miasma was the idea that diseases, most if not all of them, were caused by filth, dirt, bad air, and other factors that happened to be associated with people living in poverty and working in difficult circumstances. Public health officials, doctors, and others used the concept to explain many of the diseases that plagued large cities during the 18th and 19th centuries. But this wasn’t merely limited to cities. This same thinking was applied to malaria and many other diseases that we now know are caused by bacteria and transmitted through water or insects. Unfortunately, miasma led policy makers to make disastrous decisions that cost many lives.
How did this thinking lead to the deaths of thousands? As Johnson documents, miasma dominated the thinking of well intentioned public health officials who looked at London in the 1840’s and 50’s and saw cesspools and human excrement all across the city. The leading public health official of the era, Edwin Chadwick, went to his grave believing that the smells and poor quality of the air that resulted from these huge collections of human waste were the main cause of disease and death. Chadwick and other progressive reformers were determined to eliminate the smells by moving the waste through the construction of a sewer system into the river Thames, which was also the main water supply for the city. This caused cholera outbreaks to become more frequent. Despite good intentions, their actions led to countless more deaths.
How deadly was cholera during this period? Johnson provides some context today and is particularly relevant and chilling when he writes:
At the height of a nineteenth-century cholera outbreak, a thousand Londoners would often die of the disease in a matter of weeks – out of a population that was a quarter the size of modern New York. Imagine the terror and panic if a biological attack killed four thousand otherwise healthy New Yorkers over a twenty day period.
To overcome this deadly and well-intentioned bias, the scientific community needed individuals who were unwilling to let the common prejudices of the day dominate their thinking. They needed, as Johnson noted, someone well-practiced in consilience. Consilience is the principle that when we use independent, unrelated sources we can draw stronger conclusions, particularly about science. Thus, consilience forces investigators to use induction from the evidence, not let the dominant paradigm structure their thinking. There was just such a pair of individuals at London in the 1850s, a young Anglican priest, Henry Whitehead and one of England’s leading medical minds Henry Snow.
Both Whitehead and Snow were openly contrarian thinkers who were drawn toward evidence based approaches to solving problems. Johnson writes that Whitehead often said to people “Mind you, the man who is in the minority of one is almost sure to be in the right.” Snow was no less willing to buck the conventional wisdom. He almost single-handedly introduced the safe and effective use of first ether and later chloroform as anesthetics in English medicine.
Through his mastery of anesthetic, Snow had reached the pinnacle of the medical profession. He had administered chloroform to Queen Victoria to help ease the birth of her eighth child, Leopold. He was widely respected and had risen from humble origins to be one of the leading physicians in London. And discovering the cause of cholera was a side interest of his practice. He began collecting data from various cholera outbreaks working under the theory that the disease was carried by water trying to disprove the miasma view of the spread of the disease, in one case visiting the home of lower class Londoners in rough neighborhoods to try to show that their water was the cause of the disease. The mainstream medical community always found ways to avoid accepting Snow’s results, but he persisted.
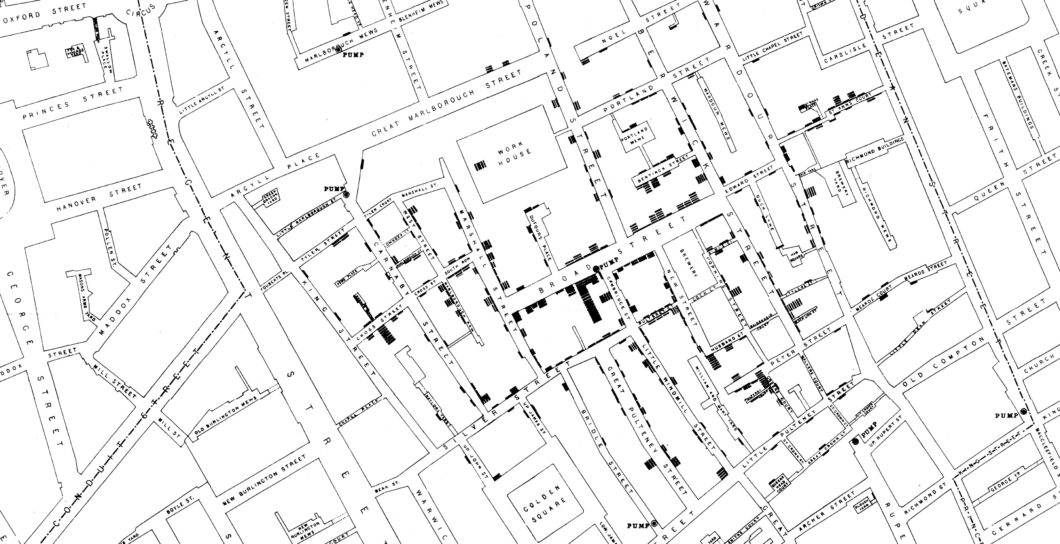
When the most devastating outbreak struck in 1854, it was located in one specific neighborhood that predominantly relied on water from the so-called Broad Street well. Whitehead was then working in the local parish and witnessed the widespread death of many of his parishioners from the disease. He and Snow investigated independently at first, but later working together, combed the neighborhood interviewing virtually every family in the area. Their work showed convincingly that those who drank from the Broad Street tap became sick and many died from the water. Those who drew their water from elsewhere did not. They managed to overcome the bias towards miasma, only through the overwhelming nature of the evidence and the pump that drew water from the Broad Street well was shut down. It turned out tragically that the cesspool that was later shown to have contaminated the tap water was that of a family with a young baby daughter who died of the disease. Her mother had been discarding the child’s waste in the cesspool in front of her home and this inadvertently led to the child’s death.
After the closing of the Broad Street well did the public health community abandon the concept of miasma? Did they wholeheartedly embrace the idea that cholera and many diseases could be transmitted through water? They did not. Even though they supported closing the well based on Snow’s evidence, in their final report they still attributed the outbreak to an atmosphere (not a water supply) that was “offensive with effluvia from ill-conditioned sewers; the houses were almost universally affected in the same manner” along with blaming the architecture creating bad air flow. They still believed in miasma. Writing of the report issued by the committee, Johnson himself acknowledges this, but he is careful in his assessment of their work to not indict their intentions: “They were not hacks, working surreptitiously for Victorian special-interest groups. They were not blinded by politics or personal ambition. They were blinded by an idea.”
It would be ridiculous to suggest that we are approaching the fight against Covid-19 with outlooks and perspectives that are as primitive as the one that scientists and physicians were employing during the cholera outbreaks of the 1850’s. However, we are still human, and our biases and need to use paradigmatic thinking remain. We should also remember that failed paradigms don’t die quickly or without struggle. The ability to think unconventionally and look clearly at what the data are telling us is rare. It is much easier to simply fall back on the same approaches and explanations that have been produced out of our prior biases and the existing ways of thinking. Covid-19 may not lead to the same revolutionary advances as the discovery of waterborne disease, but it clearly has provided a powerful challenge to the existing research on viruses.
Until we know more and can look clearly at what we will know in the future, we will probably continue to struggle with the disease because of what we do not yet know. Our paradigms may need to change in profound ways in the future. History will look back on this period, perhaps much as we do now at the 1850’s and marvel at how little we knew then. Science is a powerful tool for humans to make their world better, but it is not omniscient because it is the result of human action. This is particularly true when paradigms shift, which they always will. The costs for new paradigmatic thinking can be enormous. Let’s hope the price we pay for this possible change will be limited and quickly adopted.